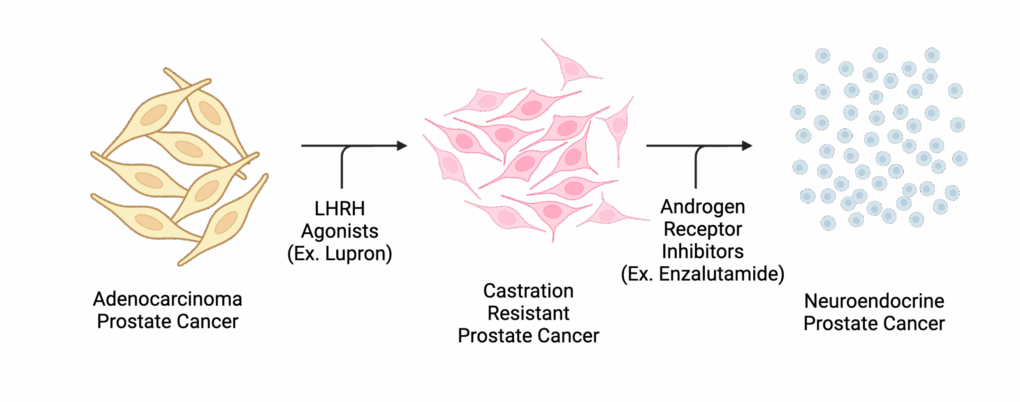
My name is Jeffery Martin, and I am a second-year Master’s student working on the prostate cancer project in Dr. Porter’s lab in the Biomedical Science Department at the University of Windsor. In honour of Prostate Cancer Awareness Month, I would like to share some of the exciting prostate cancer research happening at the University of Windsor! Prostate cancer is the second most common cancer in men worldwide, affecting 76 men daily in Canada (Canadian Cancer Society). Disease management and overall patient outcomes have improved as treatment options continue to evolve, and while effective in many cases, these treatments can sometimes pressure prostate cancer cells to change into a more aggressive type of cancer, known as Neuroendocrine Prostate Cancer (NEPC). NEPC can metastasize to other parts of the body, making the current treatments available for prostate cancer much more challenging. Our research focuses on studying the progression of early-stage prostate cancer adenocarcinoma to advanced NEPC and understanding the mechanism of the cell cycle’s regulation in this process.
We believe that through better understanding prostate cancer progression and the cell cycle’s role in this process, we will become more informed on potential treatment options. As a result of our findings, we are now testing selected drugs on prostate cancer cells to try to develop novel therapeutics that can treat and prevent the progression of prostate cancer.
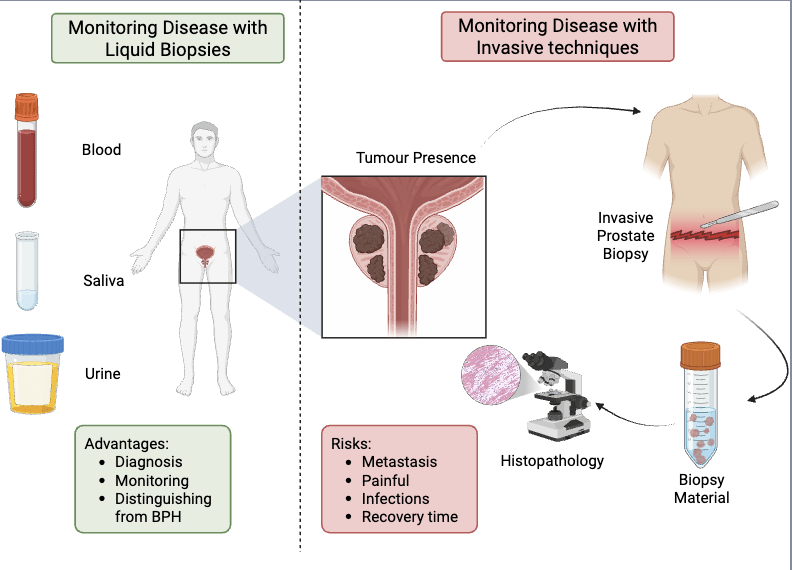
Additionally, we are also looking for novel biomarkers that can detect prostate cancer progression, and we are using non-invasive liquid biopsies to do so! Biomarkers are measurable indicators, like genes or proteins found within the body, that reveal a biological process or disease within the body. Common biomarkers for prostate cancer include PSA (prostate-specific antigen), PSMA (prostate-specific membrane antigen), and AR (androgen receptor). Although these markers are very effective at detecting early stages of cancer, unfortunately, as the disease progresses, these markers are often lost. This leads to the need for the development of new biomarkers to track disease progression.
Further, we hope to find biomarkers that can be detected in early stages of prostate cancer and indicate whether or not disease progression is expected. This would help to guide treatment plans and create a more personalized medicine approach going forward. As mentioned, we plan to use non-invasive liquid biopsies instead of traditional biopsies to detect these biomarkers. Although they are effective, traditional biopsies are invasive, painful for patients, and can lead to potential risks down the road. With liquid biopsies, we can detect these biomarkers in a less invasive way by using a blood, urine, or saliva sample. Through a collaboration with Dr. Kanjeekal at Windsor Regional Hospital, we will be searching for these new biomarkers with liquid biopsies collected from prostate cancer patients.

The research we conduct is mainly done in vitro, which means it’s done in a controlled environment, like in a test tube, instead of a living organism. Specifically, we work in a cell culture room for a lot of our experiments. At the moment, I’m working with 4 different prostate cancer cell lines, which are all derived from prostate cancer patients. We use these cell lines to mimic the progression of disease, and also for drug testing to see how the cells respond to treatment.
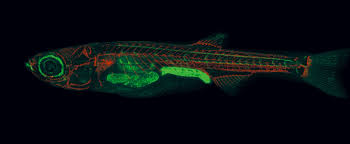
We also do some in vivo experiments, which means using living organisms. We specifically use zebrafish as a model system for testing the drugs! Using Zebrafish is becoming increasingly common around the world for drug testing and there are many benefits of this model system. First, Zebrafish are genetically similar to humans, and they are a cost-effective model that requires easy maintenance. Next, they develop quite rapidly, which is great for experimentation, and they have a transparent embryo, allowing for easy visualization. Finally, and most importantly, Zebrafish lack a functional immune system for the first 10 days of their life! This allows us to transplant human cells directly into zebrafish and then observe how these prostate cancer cells behave in a living system. From there, we can test various drugs in the Zebrafish with the prostate cancer cells and see how the cells respond to treatments in this environment. This will also help the results from our studies translate more easily and rapidly to use in humans.
This fundamental work has been supported by grants from Cancer Research Society (CRS), Ride for Dad and WE-SPARK Health Institute. Through this funding, we have made some excellent progress so far, and I look forward to the progress that we will continue to make in the upcoming years! Additionally, through submitting my project proposal to various organizations, I have been lucky enough to receive funding from NSERC (Natural Sciences and Engineering Research Council of Canada), the Windsor Prostate Cancer Scholarship, the Dr. Michael L. Petras Memorial Scholarship, and the Doctor Family Health Research Student Support Award. Each of these awards has helped fund my education and allowed me to spend more time working in the lab. Further, another Master’s student working on this project, Christian Kassa, was recently awarded a Canadian Cancer Society Research Training Award. This is a very prestigious award with only 6 recipients across all of Canada. Christian just started his graduate studies this year and will be helping advance this project over the next 2 years!

A highlight of my project has been the various connections I have made with the community and other researchers at various conferences and local events. At the WE-SPARK Health Research Conference, I had the privilege of being a LEARN program host, which stands for Lived Experience Accelerating Research Knowledge. As a LEARN host, I was paired up with two local prostate cancer survivors who were able to share their lived experiences with me and give insight into the patient perspective. Oftentimes, when working in the lab, I forget about the direct impact my work can have, and these connections remind me of the importance of research. Further, the two patient participants that I was paired with are both members of Windsor’s local Prostate Cancer Support Group, and through making a connection with them, I was invited to speak to their group this upcoming November! Presenting our important work at various conferences has attracted the interest of other researchers and physicians for possible collaborations.
It’s important to recognize everyone involved in this project as none of this work would be possible without the help of our multi-disciplinary team. This project is supervised by Principal Investigator, Dr. Lisa Porter, and Research Associates, Dr. Elizabeth Fidalgo and Dr. Bre-Anne Fifield. Our clinical collaborator is Dr. Sindu Kanjeekal, the Chief of the Department of Oncology at the Windsor Regional Cancer Centre. In-lab experiments are carried out by myself, Jeffery Martin, fellow graduate student, Christian Kassa, and undergraduate student, Kaitlin Ferraro. Previous lab work was completed by Dr. Martin Bakht while a PhD student in our lab, and undergraduate thesis student, Maria Badalova. Knowledge translation work is completed by our Clinical RA, MSc Samavia Ahmad, and Masters of Translational Health Science student, Hannah Ferasol. Finally, none of this project’s advancements would be possible without the help of everyone else in Porter lab who help to provide meaningful feedback and insights that help drive this research further.

I hope you enjoyed learning a little bit more about the prostate cancer research taking place at the University of Windsor. Feel free to watch the video here if you want to see more of the work we do. If you have any questions, please leave a comment below, and I will get back to you! And if you enjoy reading it, please share it below! Jeffery